A bus driver involved in a crash was charged with “child endangerment, driving while impaired and possession of drug paraphernalia” - "law enforcement sources have told PIX11 News that they believe" the driver "had overdosed on heroin." With an investigation underway, it will be determined soon enough whether the driver was using illegal drugs or as the owner of the bus company claims, “The sugar dropped on her...and she went into a coma” revealing that complications from diabetes and its treatments could be to blame. The notion raises a worthy reminder that all unconscious, fainting or worse episodes are not interchangeable or incited by a uniform etiology (read here to learn why we faint).
In fact, a low blood sugar as suggested here could rapidly be reversed if caught precipitously and corrected. Cardiac arrhythmias, electrolyte imbalances and seizures are among a number of conditions that can trigger abrupt changes in consciousness that imperil a driver, their passengers and others on the road.
And, with appropriate medical training, obtaining the history and performing a physical examination, a professional can often discern whether a glucose bolus or portable defibrillator are the necessary intervention. This tends to be easier in a well-stocked emergency room. At the roadside, this isn’t always the case given the limited capacity for diagnostic testing and monitoring along with lack of proper equipment - this is why, in lieu of a precise diagnosis, certain standard protocols are reflexively implemented. These include therapies whose delay could pose substantial, even irreversible damage to the person if withheld.
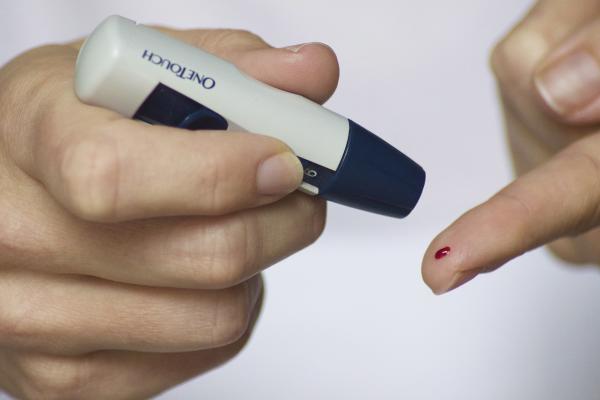
As per diabetes, there are short- and long-term consequences of the disease. Hypoglycemia, low blood sugar, is a worrisome event often caused by diabetic treatments. Extreme heat or illness and stressful periods can place a patient at particular risk compounding the problem. Sugars tend to go awry during these times and the patient must manage their medication accordingly. If a patient gets too much insulin and hasn’t eaten, for instance, then the blood sugar can plummet putting a patient in a potentially life-threatening circumstance. If mild, then a patient can sense he or she must eat to reverse the issue. In more significant cases, a patient can be unaware and lose consciousness - a diabetic coma can happen from dangerously high or low blood sugar. Additionally, depending on where the event takes place (e.g. swimming in a pool, while driving), other injuries (e.g. drowning, head trauma) can complicate things further.
In general, the more well-controlled the diabetes, the less the longer-term secondary problems or at the very least the less they have of a chance to progress. Serious irreversible damage can still result, but improving diet, not smoking, increasing physical activity, optimizing glycemic control, managing blood pressure and consistent follow-up with a medical team who can be on top of early interventions provides the most proactive means for ensuring good health and preventing worsening.
To learn more about the early signs of diabetes and the various forms, review this piece. To understand Type 1 Diabetes specifically, read here.