Supplements, currently a $30 billion industry, are the best example of “it couldn’t hurt.” A meta-analysis of meta-analyses finds, once again, that supplements have no impact on the great killer, cardiovascular disease. Published in the Annals of Internal Medicine, the study looked at randomized controlled trials (RCT) on adults estimated all-cause mortality and cardiovascular outcomes [1], written in English. The nine meta-analyses and four new RCTs remaining after narrowing the search considered 16 different supplements and eight dietary interventions involving close to 1 million people.
Here in one graphic, are the results
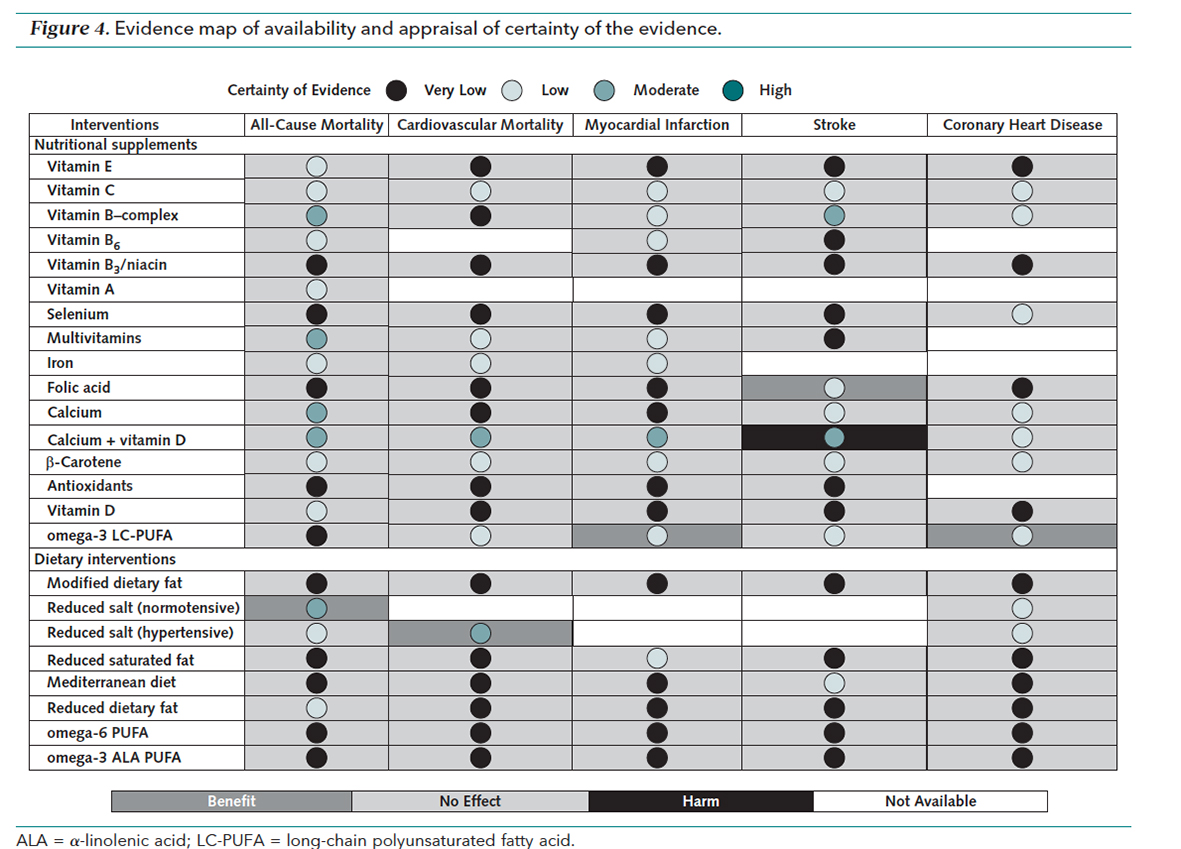
- Only reduced salt intake for patients without high blood pressure reduced the risk of all-cause mortality by 10%, with “moderate certainty.” [2]
- Only reduced salt intake for patients with high blood pressure reduced the risk of cardiovascular death by 33%, with “moderate certainty.”
- Only fish oil reduced the risk of heart attack, by 8%, with “low certainty.”
- Folic acid supplements reduced the risk of stroke by 20% with “low certainty,” while the combination of Vitamin D and calcium increased the risk of stroke by 17% with “moderate certainty.”
- Only fish oil reduced the risk of coronary artery disease, by 7%, with “low certainty.”
No study is perfect; this study is no exception. Most importantly, this looks at populations, not individuals, so yes, there will be people who may benefit from a supplement. Usually, they are individuals with deficiencies, but otherwise, it is hard to identify who is best served by taking supplements if they exist outside of anecdotes.
Salt remains problematic. As I have written previously, the effect of salt on health seems more U or J shaped than linear, too much or too little are both bad. But as the accompanying editorial for this paper points out, salt reduced all-cause mortality only for individuals without high blood pressure, while lowering coronary deaths only for people with high blood pressure. So perhaps just those individuals at real risk, those with hypertension, should watch their salt intake.
Fish oil as a supplement remains a hot mess. This study shows a very small effect with little certainty that it is correct. But a recent trial of a highly purified form of fish oil, icosapent ethyl [3], showed a 25% improvement in cardiovascular outcomes. But this is not a supplement, it is a prescribed, FDA regulated, medication; and its efficacy was shown for those patients know cardiovascular disease or diabetes, on a statin, with elevated triglycerides and involved doses of fish oil four-fold greater than found in supplements.
The finding on folate points to another problem in getting to the scientific truth about supplements, the lower risk of stroke was “largely driven” by one study in Chinese individuals with high blood pressure. This may reflect a dietary difference; there are many fewer foods fortified with folate in China than in the US, or perhaps a genetic variability. Your diet and genetics influence the effect of supplements – put another way; if your dietary need is greater than your intake, correcting the imbalance is helpful.
Finally, multivitamins and dietary interventions adjusting the type and amount of fats eaten had no benefit.
The accompanying editorial makes several important points; this is, in my opinion, the most salient
“Only recently with machine learning of large data sets, which include multimodal data on physical activity, sleep, medications, demographic characteristics, intake and timing of all foods and beverages, and gut microbiome constituents, have we begun to learn that the use of any specific diet or supplement is likely to have markedly heterogeneous effects. Testing any diet or supplement in a broad population without acknowledging interindividual variability seems like a recipe for failure, especially because most trials are not randomized, are not of sufficient duration, or do not have enough hard outcome events.” Emphasis added
There is no magic supplement, no superfood, no ancient secret hidden by unscrupulous capitalists. You need a diet that supplies all your needs, needs that change over time. The most common problem for precision health to address is diet, not treating disease. We spend over $350 a year [4] on supplements, a quarter of what we spend on out-of-pocket pharmaceuticals. If you want to lower your out-of-pocket health costs, stop taking supplements, there is just no good evidence that they help; and “that it couldn’t hurt” seems like such a poor reason to spend money.
[1] Heart attack, stroke or coronary artery disease
[2] “We are moderately confident in the effect estimate: The true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different.”
[3] It is fish oil that lowers triglycerides while not causing an increase in LDL. The manufacturers, unsurprisingly, take great effort in characterizing their product as far different from fish oil supplements.
[4] Americans Spend $30 Billion a Year Out-of-Pocket on Complementary Health Approaches, National Institute of Health
Source: Effects of Nutritional Supplements and Dietary Interventions on Cardiovascular Outcomes Annals of Internal Medicine DOI: 10.7236/M19-0341




