It's a new week, and a new dietary study. This is from the Lancet, and it is a two-year randomized control trial of calorie restriction. Calorie restriction has many meanings of late, do you restrict how the number of calories, when they are consumed, or some combination? This research looks simply at reducing the number of calories consumed compared to the control groups, "eat whatever you want," diet. And it looks at healthy young to middle-age adults with a BMI of 25, just “outside” the range considered healthy.
Participants [1], predominantly Caucasian women, age 38, began with a 4-week educational program and were all fed three standardized meals a day so that their metabolic rate and calorie needs could be calculated as accurately as possible. They were then randomized and followed for two years, which is considered a mid-term study length. Their dietary choices were tracked through 6-day food journals; they received weekly individual and group counseling sessions during the first six months and compliance with calorie restriction determined by weight loss along a predetermined “trajectory.” Of course, these are not conditions we will see in the real world soon, so apply how many grains of salt as you want to their results.
The outcomes were not health outcomes, but biomarkers; including blood pressure, lipid and glucose profiles, C-reactive protein, and a score for “metabolic syndrome.” [2] 80% of the calorie-restricted group and 70% of the control group completed the study.
- The calorie-restricted group reduced their calories by 279/day at one year and 216/day at year two. The controls reduced their intake by 83 calories/day at one year and 121/day at year two.
- The calorie-restricted group had 11.9% fewer calories, based upon body weight; the control, virtually unchanged. In terms of weight, calorie restriction resulted in an 8.4kg loss in year one, with a slight regression towards their old weight of .9kg at year two. There was no change in the control group.
- Total cholesterol, LDL, HDL, triglycerides, blood pressure, insulin resistance, fasting glucose were all improved in the calorie-restricted group, but not in the control group. The same was also true for C-reactive protein and metabolic syndrome score.
Here is the graphic:
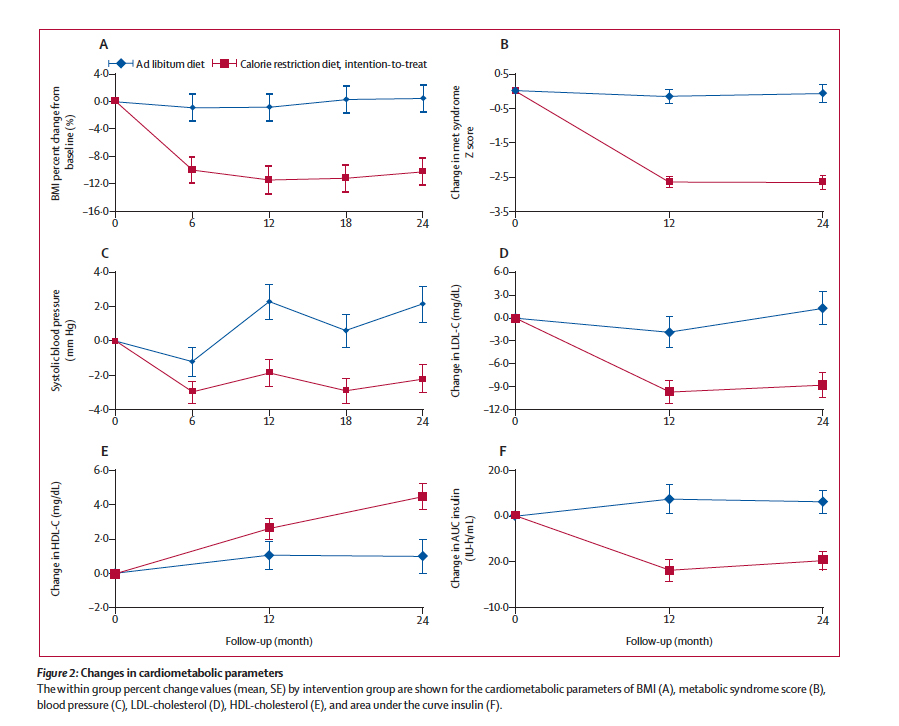
And while the researchers indicated that there were no differences in adverse effects between the two groups, the additional data they report suggests that calorie restriction resulted in more bone loss and anemia and they recommend that these conditions should be monitored.
The researchers report that calorie restriction, with adequate nutrition, improves a range of biomarkers associated with increased cardiovascular risk. Fair enough, and it is interesting to see this kind of change in individuals we would ordinarily not consider at risk at all. So in many ways, you are what you eat. What the study has not shown is that calorie restriction improves your phenotypic health, the diseases you accumulate over time. But that is the study's insinuation.
A few other thoughts come to mind. These were highly motivated individuals, and it seems that weight guidelines are a good measure for all of us to use. But notice, that the diets were not low this or that, they were just fewer calories; it makes you wonder whether our dietary choices are less critical than our caloric intake. In may not be the Big Mac that kills you as much as thinking that you can also have another meal or two that day. Another factor to consider was that the caloric restriction was targeted at 25%, but was, in the experience of a very motivated group of participants only around 11% - so extreme calorie restriction is probably not practical, and may very well be unnecessary.
[1] The 220 participants were drawn from over 10,000 volunteers with 80% removed because they were not in the target age, BMI, had medical concerns or were unable to participate in the program fully. These participants are not the general public.
[2] Metabolic syndrome is a clustering of hyperglycemia/insulin resistance, obesity, and dyslipidemia found to be a risk factor for cardiovascular disease.
Source: 2 years of calorie restriction and cardiometabolic risk (CALERIE): exploratory outcomes of a multicentre, phase 2, randomised controlled trial The Lancet DOI: 10.1016/S2213-8587(19)30151-2




