Two new studies, one surgical, the other medical come to similar conclusions - significant weight loss alters the course of Type 2 diabetes.
In the first study, 867 40 to 69-year-old, patients with new-onset diabetes were randomized into treatment or control groups. Seven hundred thirty had both their weights and HbA1c measured initially and at five years and represented the study group. It was predominately Caucasian (97%), male (61%), and with a BMI of about 34. At the end of 5-years, 30% of patients who lost 10% or more of their body were in remission from diabetes. And the incidence of remission followed the degree of weight loss – the kind of dose-response to treatment that suggests underlying physiologic changes. The researchers considered several associated behavioral changes, smoking cessation, less alcohol or caloric intake, fewer fats, more exercise, you know the litany. But with the exception of a small improvement with diminished alcohol intake, none of those changes made a difference – it was solely that drop in weight.
"These findings suggest that remission is achievable without intensive lifestyle interventions or extreme calorie restrictions."
Of course, the study has some fine print. First, while a weight loss of this magnitude during the five years achieved this result for some patients, it was more effective earlier in the course of the disease. The more important caveat and one many of us know first-hand, losing that amount of weight and keeping it off is far easier said than done. And that brings us to the second study.
When is a "bug" a feature?
One of the most frequently performed operations in the mid-20th century was a host of procedures for treating peptic ulcers, stomach ulcers. They have been substantially entirely supplanted by medications like ranitidine (Zantac currently under recall). But even though all those different operations on the stomach "cured" the ulcers, many had an adverse side effect, significant weight loss. Innovative surgeons turned that adverse effect, that operative "bug" into an operative benefit with the introduction of bariatric surgery – alterations of the GI tract meant to reduce a patient's weight.
There are several operations categorized as bariatric surgery, some designed to diminish the size of the stomach, increasing the onset of satiety and reducing caloric intake; others that re-arrange the GI tract to reduce capacity and alter metabolism. All are associated with significant weight reduction and have been offered to patients who are significantly obese. A new study looks at how patients, with Type 2 diabetes, undergoing bariatric procedures fare for adverse cardiovascular outcomes – the usual concerns of heart attacks, strokes, and other problems.
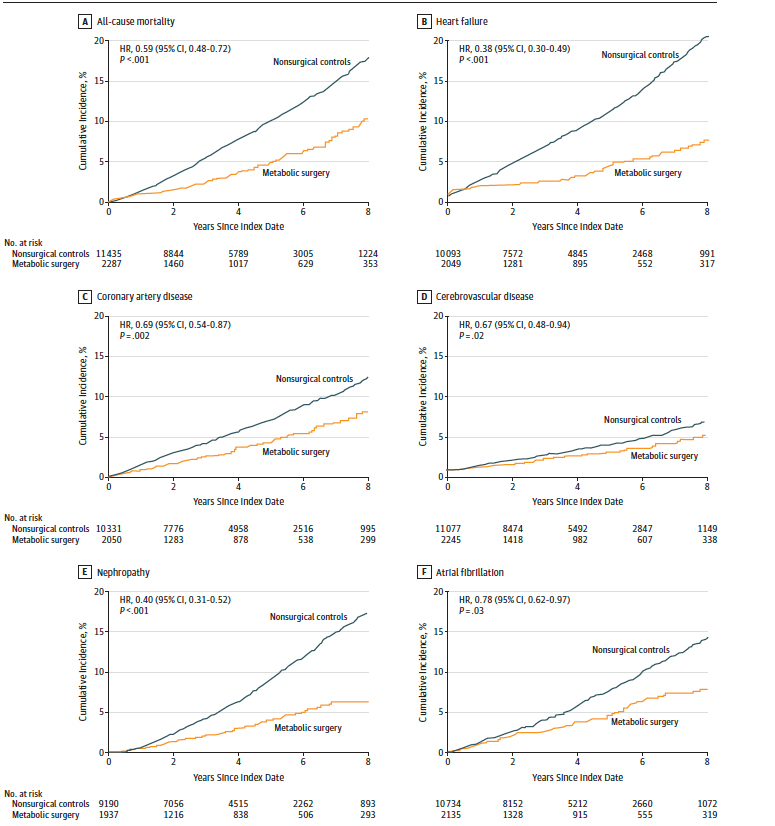
Roughly 2300 patients undergoing bariatric surgery and with a history of Type 2 diabetes were followed for approximately four years and compared with control patients who did not undergo bariatric surgery. An inspection of the two groups suggests that the control patients were at best "similar" rather than the same, so the effect size I am reporting should be taken with a grain of salt. These patients were far more overweight at a BMI of 40 or higher than the previous study. The surgical group had more dyslipidemia and hypertension; the control group more smokers and blacks. The cumulative incidence of all-cause mortality, coronary artery disease, heart failure, cerebrovascular disease (strokes) atrial fibrillation, and nephropathy (kidney disease) were all reduced over the 8-year follow up for the surgical patients as compared to the controls.
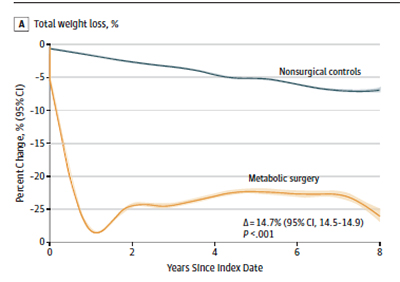 But for me, the critical finding is the profound and long-standing weight loss from the surgery, as depicted on the right. These patients not only had remission from diabetes but significant reductions in the need for medications for both hypertension and dyslipidemia.
But for me, the critical finding is the profound and long-standing weight loss from the surgery, as depicted on the right. These patients not only had remission from diabetes but significant reductions in the need for medications for both hypertension and dyslipidemia.
"We speculate that the lower rate of MACE after metabolic surgery observed in this study may be related to substantial and sustained weight loss with subsequent improvement in metabolic, structural, hemodynamic, and neurohormonal abnormalities."
The surgery is not a free ride, as with all procedures, there can and were complications; 0.7 % of patients died within 90 days of surgery (for open-heart surgery that percentage is about 3.7%). Five percent needed open surgical revision, while 16% had revisions of their operation by more non-invasive means. The authors are not suggesting that bariatric surgery be the primary treatment.
What I think is clear is that in well-motivated patients, a 10% weight loss can "reverse" Type 2 diabetes and show significant improvements in many associated cardiovascular diseases. And weight loss, whether or not assisted by bariatric surgery, had a more substantial impact on adverse cardiovascular outcomes than the new generation of medications for diabetes advertised with an "added cardiovascular benefit." The signal from the studies is strong; at least for me, losing a significant amount of your "over" weight is strong medicine.
Source: Behaviour change, weight loss and remission of Type 2 diabetes: a community‐based prospective cohort study Diabetic Medicine DOI:10.1111/dme.14122 and Association of Metabolic Surgery With Major Adverse Cardiovascular Outcomes in Patients With Type 2 Diabetes and Obesity JAMA DOI: 10.1001/jama.2019.14231




