Until the arrival of the GLP-1 medications, bariatric surgery was the most effective means of reducing and maintaining weight loss.
bariatric surgery
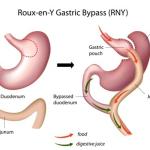
There are several ways to rearrange the stomach to caused weight reduction.
Two new studies, one surgical, the other medical come to similar conclusions - significant weight loss alters the course of Type 2 diabetes.
Severe obesity (BMI = or > 40, or 35 if there are coincident health conditions) carries with it a variety of increased health risks, such as for type 2 diabetes, high blood pressure, and heart problems.
For the extremely obese (i.e., those with a BMI over 40), the most effective means of losing weight and keeping it off is bariatric surgery — as we have di
Bariatric surgery, as we've noted before, is currently the most effective way to deal with extreme obesity.
We've discussed the benefits of bariatric surgery (for different types, see here) for the obese with or without diabetes, and at this point it's been widely accepted that th
Type 2 Diabetes (T2D) used to be called "adult-onset" diabetes because it was typically seen in people aged 40 and up, as opposed to Type 1 which is frequently seen in younger folks — even children.
Bariatric (weight loss) surgery works. A severely obese person (BMI > 40) might lose 50 percent of his or her excess body fat in the first year after such surgery.