Irrespective of how you feel about wearing a mask and maintaining a "social" distance, the preponderance of the evidence is that COVID-19's transmission is through the air and our breathe rather than through touch or direct contact. (That means we can wash our Amazon boxes less, and our hands more – to be on the safe side.) While there continues to be debate over the definitions of aerosols, how long they remain aloft, the impact of ventilation systems, all of which show you how little we really know about how even seasonal flu is spread, for those placing or removing breathing tubes (intubation or extubation) the respiratory source of COVID-19 is the small space where they share breathes with these patients.
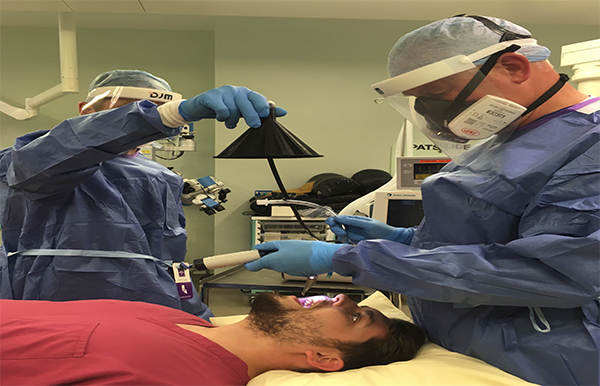 These procedures have been designated "aerosol-generating procedures." In these circumstances, appropriate protective equipment includes a fitted mask filtering 95 to 99% of the air, long-sleeve gowns, gloves, and some eye protection. While this protection level is easily achieved under elective circumstances, putting all those protections on in an emergency takes up valuable time, and continuously walking around in those outfits is more than bothersome. Like other early measures taken against COVID-19, the designation was put into place before we had any good or reliable information when an abundance of caution was necessary. This new study seeks to fill in the information gap now that we have had a chance to catch our breath.
These procedures have been designated "aerosol-generating procedures." In these circumstances, appropriate protective equipment includes a fitted mask filtering 95 to 99% of the air, long-sleeve gowns, gloves, and some eye protection. While this protection level is easily achieved under elective circumstances, putting all those protections on in an emergency takes up valuable time, and continuously walking around in those outfits is more than bothersome. Like other early measures taken against COVID-19, the designation was put into place before we had any good or reliable information when an abundance of caution was necessary. This new study seeks to fill in the information gap now that we have had a chance to catch our breath.
Aerosol-generating procedures are, by definition, more likely to produce aerosols than coughing, so researchers had a measure to use. They employed optical scanners that could count particle and their size reliably on a second by second basis. The device was positioned a little over a foot away from the patient and practitioner. The study was conducted in a room designated for these high-risk procedures where the baseline particulate matter was low enough that small changes could be identified. The study was small, looking at 38 volitional coughs, 19 patients with a breathing tube placed, and 14 patients with a breathing tube removed.
- Baseline values showed 0.4 particle/liter when the room was empty and 3.4 particles/liter when the room was in use for non-aerosol generating procedures.
- Coughs produced an average of 1310 particles/liter over a time frame that peaked 2 seconds after the cough began, returning to the baseline after 2.7 seconds. The majority of particles were smaller than 1 µm
- When inducing the intubating a patient, the average number of particles was 500-fold less than recorded for volitional coughing, and the maximum was 22-fold less.
- When extubating a patient, removing the breathing tube, the average particulate matter was 35-fold less than a volitional cough, but the maximum was, in some cases, similar to coughing. Coughing is not an uncommon event when this tube is being removed, and in those cases, particulates were about a quarter of what is seen with volitional coughing.
For my colleagues, this suggests that intubation, the procedure that is most likely to be an emergency, is safer than we expected. For extubation, the data is, in the words of the researchers, "more nuanced." The aerosols generated are greater, especially with coughing. They recommend anesthetic management to decrease the likelihood of coughing upon extubation as a mitigation strategy.
The studies were conducted in special laminar flow rooms, but similar measurements in your run-of-the-mill operating rooms produced similar values. They are quick to point out that the laminar flow environment's lower baseline particulates make it more sensitive to their identified changes. The study has other limitations beyond its small size. One might argue that the air sampling itself was insufficient or that the tested patients did not have COVID-19—all reasonable concerns.
"Importantly it should be acknowledged that we are unable to make any conclusion about the risk of actual SARS-CoV-2 transmission as aerosol generation is still only a presumed risk factor and particle number concentration is a plausible but unproven surrogate measure of that infection risk."
This study begins to shed some light on the possible degree of exposure, which is a step forward. That we have no direct measure of infectability shows you have much further is the journey. It is the same when we talk about a viral load, a concern increasingly present in the media's town square. We know that viral load correlates with infectability, but there is not a simple linear increasing relationship. For the anesthesiologists, registered nurse anesthetists, and respiratory therapists who continue as front-line, at-risk individuals, this study should provide some comfort. Still, it may not result in continuing to act out of an abundance of caution.
Source: "A quantitative evaluation of aerosol generation during tracheal intubation and extubation" Anaesthesia DOI:10.1111/anae.15292 Image is taken from article