Lead in drinking water is a practical example of a 3-legged stool. Realizing that lead pipes may have been installed in a neighborhood comprises the first leg - community-level information. Examining the pipes supplying a selected residence and measuring the drinking water’s lead content is the second leg – the local effects; cognitive testing of individual residents would be the third “individual” leg.
COVID epidemiology is the obverse of air pollution epidemiology.
Air pollution epidemiology rests on the single leg of community-level outdoor air quality for conventional air pollutants, assuming that each member is equally exposed to those substances and concentrations. With nothing known about the local (indoor) environments or the characteristics of exposed individuals, it is a shaky epidemiologic stool.
COVID epidemiology is based on tests of individuals selected by likely exposures or observed symptoms, the final individual leg of the three-legged stool. But little is known about those other legs, local and background environments. I wrote about these issues in 2020 [1]; we now have the benefit of some actual data.
An individual is both a source and a receptor for COVID. We have some understanding of viral shedding, the source, and our non-pharmacologic interventions (masks and distancing) speak to our role as COVID receptors. What can be done at the group or community level? Here I discuss both ends of the process; virus carried by the ambient air where we live and breathe; and virus levels in wastewater, accounting for where we have been.
The Air
The size distributions and concentrations of virus-laden aerosol particles released by infected individuals play 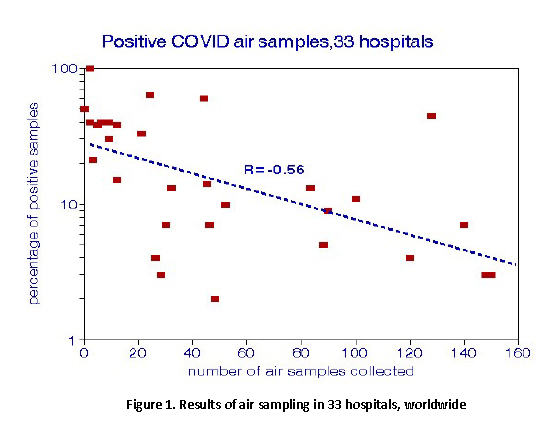 important roles in their transmission. Aerosol distributions are spatially heterogeneous and can indicate locations where individuals should be tested. Dinoi et al. reviewed and summarized air sampling data from 77 datasets, showing that a few selected samples had higher rates of positivity, more than from widespread sampling. For example, the median positivity in Figure 1 is 14%, while the national median of about 800,000 individual positivity tests was about 3% at this writing. Concentrations of SARS-CoV-2 RNA in the air were highly variable and tended to be lower outdoors than indoors; concentrations in hospitals and healthcare settings exceeded those in community settings.
important roles in their transmission. Aerosol distributions are spatially heterogeneous and can indicate locations where individuals should be tested. Dinoi et al. reviewed and summarized air sampling data from 77 datasets, showing that a few selected samples had higher rates of positivity, more than from widespread sampling. For example, the median positivity in Figure 1 is 14%, while the national median of about 800,000 individual positivity tests was about 3% at this writing. Concentrations of SARS-CoV-2 RNA in the air were highly variable and tended to be lower outdoors than indoors; concentrations in hospitals and healthcare settings exceeded those in community settings.
Wastewater
Wastewater sampling for pathogens is not new. Human-excreted substances entering a sewer system can be related to exposures of the contributing population. Wastewater analyses for COVID have been reported in California, Massachusetts, and New York, among others, and the CDC has established a data dashboard.
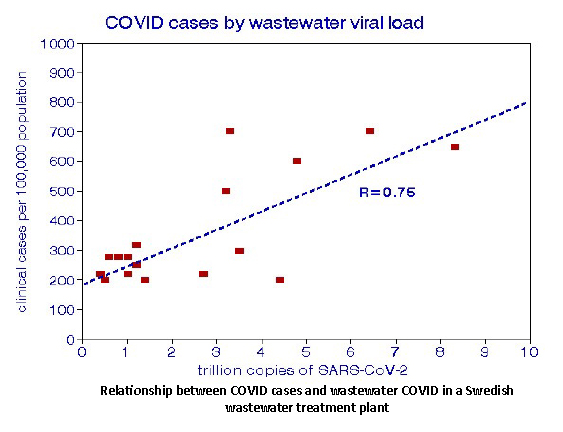 Isaksson et al. collected samples from 2 wastewater treatment plants in northern Sweden and compared virus copying with clinically determined cases. I cross-plotted the larger treatment plant data and found a potentially predictive positive correlation. One crucial factor in time-dependent analysis is the lag between cause and effect, which Isaksson et al. found to be several days. The relationship at the other Swedish treatment plant was also significant but with similar case counts at lower virus levels. This led the authors to conclude that differences among sewer catchments must be considered when developing predictive relationships. Nattino et al. found an even closer relationship between wastewater COVID and positive tests and hospitalizations in Milan over a longer period and discussed some of the difficulties in specifying relationships. Nevertheless, these experiments demonstrate that wastewater analyses can help track community-wide infection trends.
Isaksson et al. collected samples from 2 wastewater treatment plants in northern Sweden and compared virus copying with clinically determined cases. I cross-plotted the larger treatment plant data and found a potentially predictive positive correlation. One crucial factor in time-dependent analysis is the lag between cause and effect, which Isaksson et al. found to be several days. The relationship at the other Swedish treatment plant was also significant but with similar case counts at lower virus levels. This led the authors to conclude that differences among sewer catchments must be considered when developing predictive relationships. Nattino et al. found an even closer relationship between wastewater COVID and positive tests and hospitalizations in Milan over a longer period and discussed some of the difficulties in specifying relationships. Nevertheless, these experiments demonstrate that wastewater analyses can help track community-wide infection trends.
Dreaming About “Normality”: A Modest Proposal
COVID’S 3-legged stool could consist of
- monitoring community wastewater for trends
- sampling residential, hospital, or nursing home room air for localized spatial data
- conventional swab testing and symptom evaluation of individuals deemed most at risk.
Routine wastewater sampling could provide ongoing community trend information after calibration to local conditions. If a critical viral surge were detected, indoor air sampling could then identify local hot spots.
This scenario requires developing a continuously operating remote coronavirus monitoring device in the mode of a household smoke or carbon monoxide detector or a community-level ambient air quality analyzer. Such devices would be required in a nursing home or hospital setting and community facilities such as schools, theaters, sports arenas, houses of worship, etc. Given the success of last year’s “warp speed” vaccine development program and the current level of technological ingenuity, I’m hopeful that such a dream could become a reality, given adequate funding.
A remedial response to high COVID levels in room air would be to increase ventilation and/or relocate the most vulnerable residents. A widespread community infection might prompt a face mask mandate, but it would then be based on actual exposure data rather than a subjective judgment by a public health official. Community facilities would be required to demonstrate safe conditions before public attendance and monitor any subsequent changes during occupancy.
Perhaps the most valuable result from this scenario would be characterizing indoor viral conditions in terms of community vaccination coverage. Scolding the vaccine-resistant could shift from “you are a bad person” to “air in this room is not safe for your vulnerable grandmother or child,” or “sorry, tonight’s basketball game has to be canceled.”
There may be safety in numbers; let’s get started by providing data related to public safety!
[1] Coronavirus As An Air Pollutant; Towards A Better Understanding Of Coronavirus Aerosols, An Engineer’s Proposal; Coronavirus And Air Pollution, Redux.



