In the first article of this series I discussed the LAST of four measures that the Center for Medicare Services (CMS) uses to establish hospital star ratings —the patient experience, which heavily weighted in determining hospital ratings.
Patient Experience
Following discharge, a sampling of patients were asked to complete a survey, which rated various hospital measures of quality:
- Is the hospital environment, clean, quiet, and conducive to healing?
- Do nurses and doctors communicate well, how responsive is the staff to patient concerns especially pain?
- Were discharge plans and medications (two components that can adversely impact readmissions) discussed?
- Would you recommend the hospital to others?
While rated on a scale from one to five, only the response – always providing care, a five – were counted. Never, sometimes and usually providing care as patient responses did not count. The competition among hospitals is fierce, so just a few additional “5’s” can make an enormous difference in the hospital rating (1).
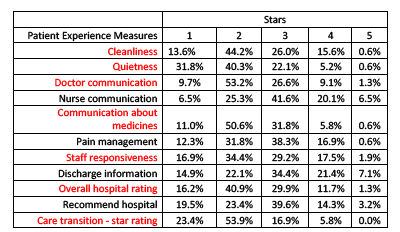
From the table above, it is clear that there is a vast disconnect between how hospitals and their staff believe they are caring for patients, and the patient’s perceptions. I have indicated in red measurements where more than 50% of patients rated their care two stars – below average. It is obvious that the majority of patients felt the care was at best, average. "Patient experience" is most likely the primary reason for the poor “star” rating of hospitals in New York State.
The other three measures, which involve time, cost, and efficiency, also reveal some interesting trends.
Effectiveness of Care
While accounting for only 4% of the star rating, effectiveness of care has eighteen separate measures:
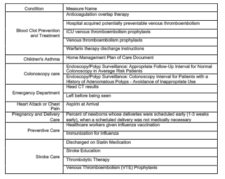

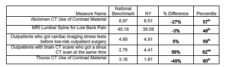
CMS reports percentage compliance with each measure, but in order to compare New York with our national benchmarks, I calculated how many hospitals were compliant for any given percentage e.g. 10% of hospitals were compliant 90% of the time. Here is an example where New York hospitals and the national benchmark were essentially the same: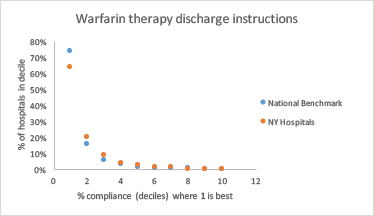
The ratings for hospitals in New York and national hospitals were nearly identical by all measures, except for timeliness of CT results (should be 45 minutes or less for patients in the Emergency Department who present with symptoms of an acute stroke). This time period is crucial because there is only a small window of time when it is possible to reverse the effects of strokes.
Timeliness of Care
How efficient is the delivery of care to patients? How quickly are patients seen, and their needs addressed? CMS measured time in managing myocardial infarctions, and caring for patients in Emergency Departments.
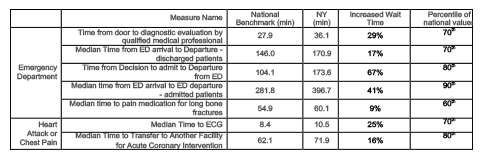
New York hospitals had significantly longer delays than national averages, and the ratings reflect this. The sheer volume of patients in the ED volume may account for some of these delays, especially in overburdened urban centers, but waiting an hour in any hospital for pain medication for a hip fracture is unacceptable.
Efficient Use of Medical Imaging
CMS has identified, in conjunction with the medical and surgical specialists, five imaging procedures that are unnecessary in specific instances, for example, an MRI of the lumbar spine for low back pain without prior conservative management.
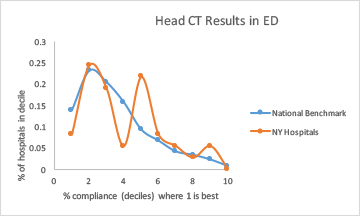
Two areas where New York's use of imaging was worse than the benchmark were stress tests and brain and sinus CTs. The pattern of usage was uneven across the state:
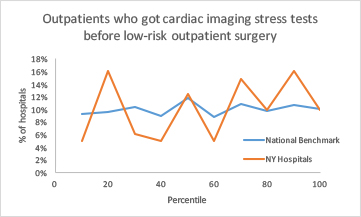
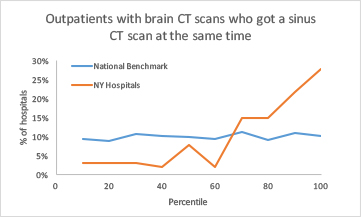
This suggests that physician education in utilizing these tests is spotty or that standardizing evidence-based testing protocols lags in some hospitals.
Conclusion
• Overall, New York hospitals, despite the reported star ratings, have low mortality rates.
• The safety of New York's patients during hospitalization can be improved, particularly with regard to surgical infections.
• New York hospitals have high readmission rates – a measure impacted by patient’s education, finances, and home-support networks. The social safety net is failing these patients.
• There is poor communication between the hospital and patients, especially with regard to post-discharge care.
• Overall, New York hospitals provide efficient, although not particularly effective care.
• New York’s hospitals have average or slightly better wait times for care when time is critical, for example, in emergency departments, and in caring for myocardial infarctions
• New York hospitals are inconsistent in avoiding unnecessary diagnostic testing
Comments
In the marketplace, reputation informs buyers and sellers. As Sy Sims put it succinctly, "An educated consumer is our best customer." (2) CMS is attempting to provide patients with that information, to inform their healthcare choices. The unfortunate assumption is that giving patients more information will overload their understanding, that a summary described as stars is adequate. As with any summary, information is lost, nuance ignored. To be fair to my physician brethren, these measures taken individually have nuanced meaning that only someone in ‘the business’ can appreciate. Not all readmissions are avoidable; high patient volumes and staffing problems prolonged wait times.
Star ratings are a first approximation. Careful analysis by hospitals and health systems can provide insight for improvement. Hospitals and their staffs need to address discharge planning and safety during hospitalization; our legislators need to begin to view our socio-demographic ills through the lens of health care costs. That the ratings are beset with problems does not mean that they should be ignored. They can and should be improved. And the truth is CMS is doing as good a job (and I think a much better job) than US News and World Report. Why is there so much controversy about CMS’s methods and so little discussion of a magazine that charges hospitals to use their ‘branding’ in advertisements?
Even with a star rating system, it is difficult for patients to choose hospitals. Physicians referred their patients to hospitals with whom they affiliate. In an emergency, you go to the closer emergency department. Star ratings will not help in those instances. But now that we have the star ratings, perhaps we can use them in different ways. How many 4 star hospitals are in insurance companies least expensive hospital networks? Can we get the leading health systems to share with those doing less well, to ensure that no patients are left behind?
Notes:
(1) This is why you always see signs at the hospital saying, “We strive for five” – a bit of subliminal advertising, which is somewhat reminiscent of reminds me of a car dealership.
(2) Sy Syms was a New York businessman who owned an eponymous clothing store with ubiquitous advertising on local television.



