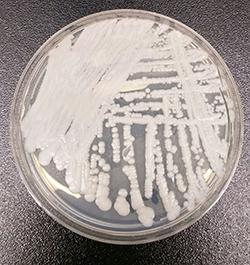
The headlines are rampant lately about “a mysterious and deadly fungal infection..spreading across the globe” that identifies multidrug-resistant yeast, Candida auris, as a “new fungal superbug.” And, as is common with such alarming headers, the proliferation of misinformation begins as well. For one, C. auris is not new having first been described in 2009 in Japan and with the earliest known infection occurring in 1996 in South Korea. So, separating fact from fiction is increasingly relevant now.



What do we know?
The U.S. Centers for Disease Control and Prevention (CDC) is considering it a “serious global health threat” because C. auris is challenging to diagnose without special technology (thereby prompting treatment delays and enhancing spread), primarily impacts health care settings and is often multidrug-resistant to commonly used antifungal medications.
For those acquiring invasive infection particularly in the bloodstream (or fungemia), there is a high mortality. Wound and ear infections are also possible, and though it has been found in respiratory and urine samples it is not clear if it causes infections in the lungs or bladder. As per the CDC, it has emerged in a number of countries for unknown reasons, and though similar within nations its strains differ between continents.
Should you worry?
Otherwise healthy people don’t have much cause for concern, but should practice infection control precautions and frequent hand-washing if a loved one is colonized (carrying C. auris on the body without causing symptoms of illness) or infected. This is always good practice, in general. How it spreads is not entirely clear, but it can be transmitted from person to person and from contaminated equipment or environments and surfaces where it can linger in healthcare settings. Though C. auris is serious for those who contract it, invasive infection is quite rare with a U.S. count of 617 cases as of the end of March.
Despite being difficult to treat as some strains are more multidrug-resistant than others, people have survived and can be treated. According to the CDC, 30–60% of those who contract it have died; however, these numbers reflect those already sick with significant diseases that also have high risks of death.
Who is at risk? And Why?
Those most at risk tend to be the most vulnerable. Individuals with multiple medical conditions who are admitted to the hospital or long-term skilled nursing facilities. Therefore, post-surgical patients, those with diabetes and recent use of antibiotics and antifungal medications are susceptible. The greatest risk includes patients with central venous catheters, tubes and lines going into the body.
The why has much to do with weakened immunity and the complicating cascade of managing those with significant disease in the hospitalized setting, especially with increased passage of time. The stress of a lengthy stay does not do wonders for the body, in fact it further impedes a person’s ability to fight infection. For example, those with diabetes have impaired wound healing and depending on the brittle nature of their disease for those with poor glycemic control a constellation of issues arise the longer they remain admitted. Many in later stages require dialysis for advanced kidney damage. These individuals routinely require invasive procedures to access their blood vessels to deliver effective treatment. To understand the many complications of diabetes and its causes, see here.
People with serious conditions warrant constant intravenous access, for instance, for blood draws and medication administration. Each time these events occur, there is an opportunity for bugs on the skin or body fluids to contaminate the situation and provide an avenue for infection. Now, sterile procedures do reduce these possibilities, but the complex often chaotic nature of the hospital setting does not bring the likelihood to zero. For those known to remain longer in the hospital, more long-term solutions for intravenous access come into play. Some get ports or other central catheters that get placed in high real estate areas like the anterior chest wall not far from the heart. Any introduction of infection into these crucial lines can be profoundly risky. Patients needing breathing assistance with ventilators are already compromised, so additional stressors worsen the scenario.
Bottom Line
The bottom line is infection control prevention should always be applied, especially in a hospitalized or equivalent environment and during patient transport between institutions. Now that awareness of C. auris is becoming more mainstream and we know of the hotspots (ie New Jersey, New York City area and Chicago), more rapid detection or at least consideration of testing should help curtail outbreaks. Improved access to specialty technology for evaluation when C. auris is in the differential diagnosis should also reduce misidentification, thereby optimizing treatment. Judicious use of antifungals might also contribute to truncating evolving these emerging infections (see here and here).
That said, hypervigilance in care of those most susceptible like individuals on chemotherapy or alternative immunosuppressed condition is of critical import. Following contact and necessary precautions can be lifesaving. To learn more about hospital-acquired infection, read here.