
The third season of The Pitt just concluded with episode 15, which may or may not have sucked, depending on your tolerance for gratuitous gore and screeching karaoke singers at the end [1]. Although episode 15 was a gross-out parade, of all the disgusting things I watched, perhaps nothing was worse than episode 8, where a woman came in with a rash so vile that I had to look away.
The diagnosis was phytophotodermatitis, aka margarita dermatitis, a condition that gets its name from bartenders handling limes and then getting some sun.
This topic is also relevant: we’re just 30 days away from May 26 (Memorial Day), the official start of the 2026 drinking season, when margaritas will be consumed in heroic quantities. (FYI, the previous drinking season will end on May 25 at midnight.)
What's up with the rash? Let's bring in the pros
The chemistry behind the rash is fascinating. And, speaking of the devil, we happen to have on staff—along with our usual collection of odd creatures—two experts in burns: Steve and Irving, your toasty hosts of the Dreaded Chemistry Lesson From Hell™. Instead of their usual venue, they took an Uber from Hell to Karaoke Night at the Downtown Cleveland Holiday Inn—a lateral move at best. Irving blew a 0.24, but his hosting duties remain unaffected.

Steve and Irving, completely wasted, at Karaoke Night at the Cleveland Holiday Inn. Not as great as it sounds.
Psoralens are therapeutic
The peels of citrus fruits contain a family of chemicals called psoralens. They do so for the same biochemical reason that bartenders get margarita rash: protection from insects. The most biologically important of these are bergamottin and 8-methoxypsoralen (8-MOP), also known as xanthotoxin.
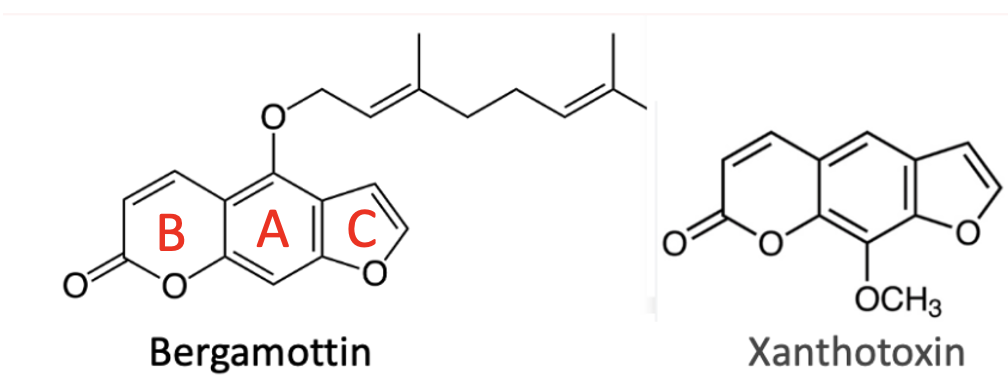
Figure 1. In psoralens, the A ring is the central benzene ring, the B ring is the pyrone (lactone), and the C ring is the fused furan ring. Don't ask.
Bergamottin (found mostly in grapefruit) and xanthotoxin are two of the most important psoralens. Xanthotoxin is an approved drug marketed as methoxsalen; in conjunction with UV light, it has long been used to treat psoriasis and eczema, although it has largely been supplanted by safer, more effective modern targeted therapies [2,3,4]. How does it work?
Xanthotoxin (methoxsalen) treats psoriasis and eczema by intercalating into DNA and, when activated by UV light, forming crosslinks that preferentially inhibit rapidly dividing skin cells—the hallmark of psoriasis. It may seem strange that this is the same fundamental mechanism as margarita rash; the difference is that in the clinic, the damage is controlled and therapeutic, rather than accidental and painful. It is no accident that the names psoralen and psoriasis are similar: both are derived from the Greek word psōra, meaning itchy, scaly skin.
Triple whammy: Intercalation meets light
Psoralens are exquisitely suited to bind DNA. This process is called intercalation. 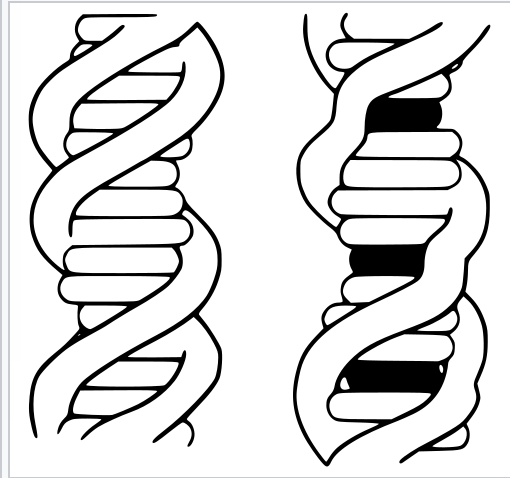
(Left) DNA strand. (Right) DNA strand with an intercalating agent inserted.
Intercalating agents bind to DNA because:
- They are flat and rigid, allowing them to slide between base pairs
- Their aromatic rings stack with the bases—like an Oreo—stabilizing them inside the helix (this interaction, known as π-stacking, is beyond the scope of this article)
- The DNA helix holds them in a specific position, aligning them for what comes next
Psoralens have all of these properties, which is why they intercalate so effectively into DNA—and why they can be so damaging.
Here's the process:
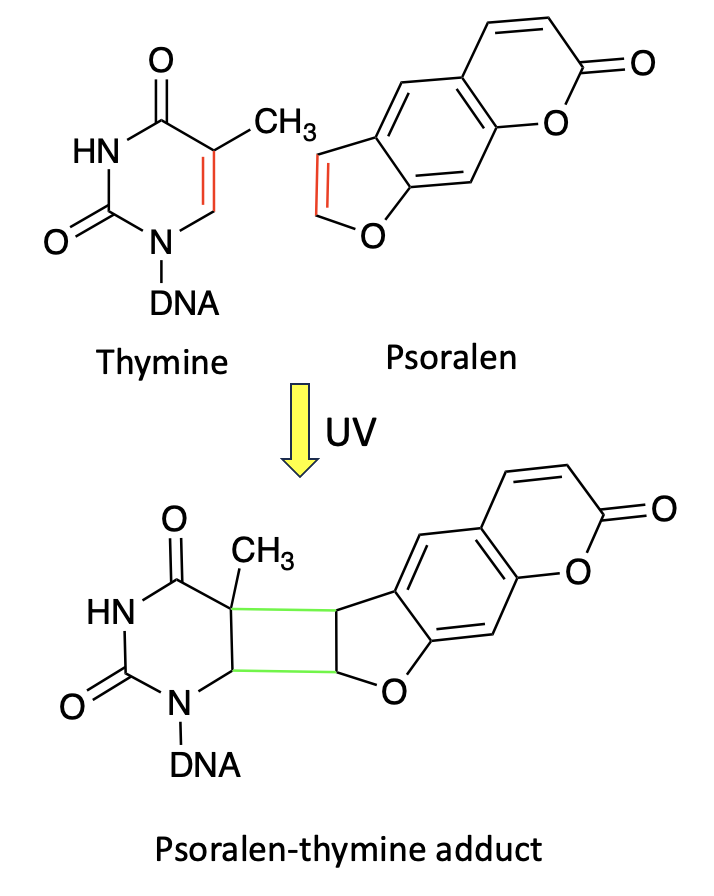
Figure 2. Intercalation and cycloaddition
- Psoralen intercalates into a thymine-containing DNA fragment [5]
- The molecule is held at a precise distance and orientation for a potential chemical reaction
- Upon exposure to UV light, the two undergo a [2+2] cycloaddition reaction (my apologies), forming a (stable) cyclobutane ring.
- A covalent bond forms between psoralen and DNA
- The result is an irreversible DNA adduct.
Then it gets worse (Figure 3).
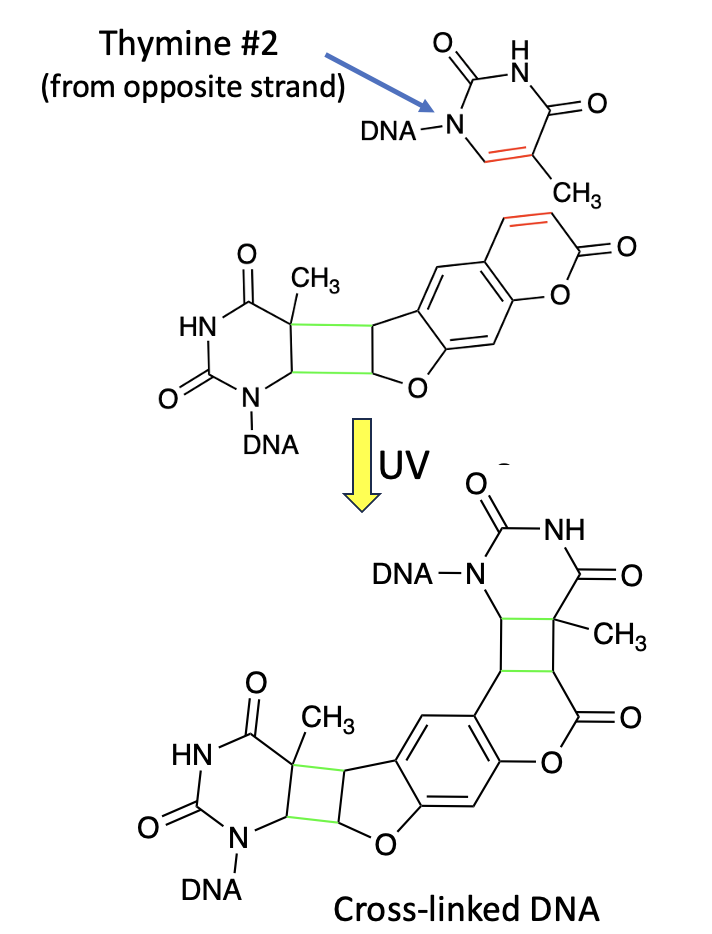
Figure 3. Crosslinking
- The psoralen-DNA adduct formed in Figure 2 is now set up so that a double bond in the B ring undergoes the same cycloaddition reaction.
- This results in a crosslink between the two strands of DNA
- The damage to DNA is now far more severe because the strands are effectively locked together, preventing normal replication and transcription and hindering the repair processes that would normally remove the lesion.
- The DNA damage kills skin cells, triggering inflammation and causing the upper layers of the skin to separate and fill with fluid—forming blisters.
- You watch episode 8 and get grossed out.
Now the process is complete:
UV + psoralen → DNA crosslinks → cell death → inflammation → blister
Extra knowledge (for those of you who are still alive)
Why has nature created such an elaborate process? Plants evolved to make these chemicals because insects also have DNA. An insect that eats a psoralen-producing plant is going to be seriously dead when the sun comes out.
Bottom line
Nature does some amazing things, like creating a family of light-activated toxins millions of years ago that makes it onto a great TV series and screws with bartenders who are only doing their jobs of squeezing limes in an effort to further intoxicate a bunch of drunks.
NOTES:
[1] Could they possibly come up with a worse ending? Stuuuuuuupid.
[2] For those who automatically demonize drug companies, consider this: psoriasis and eczema—two profoundly miserable conditions (Notes 3 and 4)—are now often well controlled with modern targeted therapies. The companies that developed these treatments have made a HUGE difference in the lives of many patients. I know this because I'm one of them.
[3] Psoriasis is a thoroughly nasty condition that can make life miserable for those who have it, causing persistent, itchy, and often highly visible skin lesions. Prior to modern immune-based therapies, treatment options were limited and often harsh. The treatments (called PUVA or psoralen-UVA) sometimes worked—but not reliably, not conveniently, and often not for long. The same DNA damage that made them work also increased the risk of skin cancer. PUVA hasn’t disappeared—but it’s mostly been pushed aside by safer, more precise treatments.
[4] Eczema was pretty awful as well, often leaving people with intensely itchy, inflamed skin that could be just as miserable as psoriasis. It was typically treated with topical steroids, which might or might not help, and came with tradeoffs such as skin thinning and, in some cases, systemic absorption, which can lead to side effects such as suppression of the body’s natural steroid production and, in rare cases, more serious effects like osteoporosis or diabetes.
That's two absolutely miserable conditions that are now generally well controlled, if not eliminated entirely.
[5] There is a reason that thymine is the preferred base. I just don't feel like explaining it.



